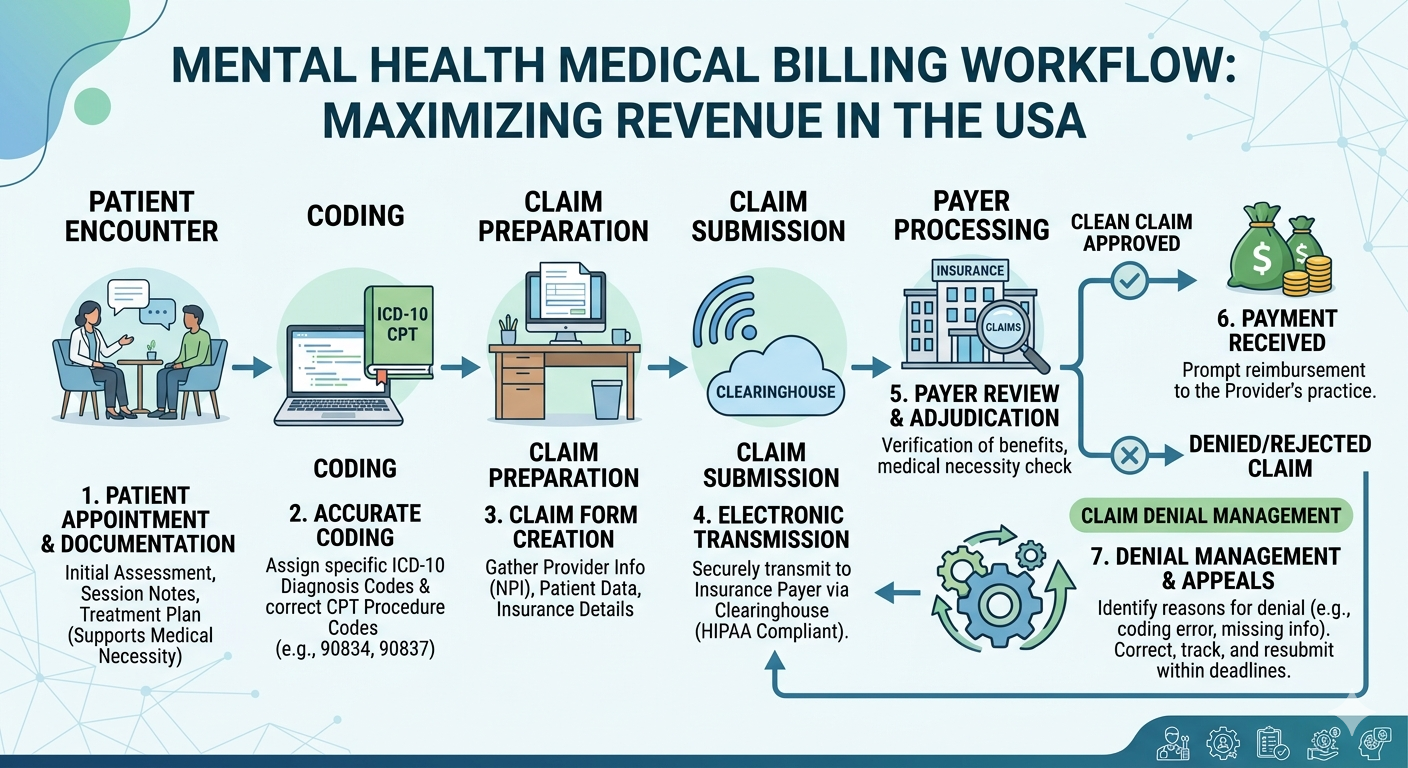
Mental health practices in Columbus are growing rapidly, but so are the complexities of billing and reimbursement. From evolving insurance policies to strict compliance requirements, providers often find themselves overwhelmed. This is where a structured approach to mental health billing Columbus becomes essential for financial stability and long-term growth.
A well-managed billing system not only ensures timely payments but also reduces administrative burden, allowing providers to focus on patient care. In this guide, we’ll break down everything you need to know about optimizing billing processes, avoiding common mistakes, and choosing the right support for your practice.
Why Mental Health Billing in Columbus Requires Special Attention
Mental health billing differs significantly from general medical billing. It involves unique coding standards, session-based billing, and strict documentation requirements. Practices dealing with mental health billing Columbus ohio often encounter challenges such as:
-
Complex CPT and ICD coding requirements
-
Frequent insurance claim denials
-
Prior authorization delays
-
Compliance with state and federal regulations
-
Managing patient eligibility and benefits
Unlike general billing, even small documentation errors can lead to claim rejections. That’s why having a streamlined process is critical.
Key Components of an Efficient Mental Health Billing System
To build a strong billing foundation, providers must focus on these essential elements:
Accurate Patient Information Collection
Collecting correct patient demographics and insurance details at the first interaction helps prevent claim rejections later.
Insurance Verification and Authorization
Verifying coverage before appointments ensures that services are billable and reduces unexpected denials.
Precise Coding and Documentation
Using correct CPT and ICD codes is crucial. Errors in coding are one of the main reasons claims are rejected in mental health billing ohio.
Timely Claim Submission
Submitting claims quickly improves cash flow and reduces delays in reimbursement.
Denial Management and Follow-Up
A proactive approach to handling denied claims ensures faster resolution and improved revenue.
Common Challenges in Mental Health Billing
Even experienced providers face obstacles in billing operations. Some of the most common issues include:
High Denial Rates
Incorrect coding, missing documentation, or eligibility issues can lead to frequent denials.
Changing Regulations
Billing requirements often change, especially in mental health billing massachusetts, mental health billing in chicago, and mental health billing in san diego, where compliance standards can vary.
Time-Consuming Administrative Work
Handling billing in-house takes time away from patient care and can lead to staff burnout.
Inconsistent Cash Flow
Delayed payments affect financial planning and overall business growth.
Benefits of Outsourcing Mental Health Billing Services
Outsourcing has become a preferred solution for many providers across the United States. Whether it’s a small clinic or a large practice, working with experts can significantly improve efficiency.
Improved Revenue Cycle Management
Professional billing teams ensure faster claim processing and reduced denials.
Cost Efficiency
Hiring an in-house team can be expensive. Many practices consider options like a cheap mental health billing company virginia or a cheap mental health billing company south carolina to reduce operational costs.
Access to Expertise
Experienced billing companies stay updated with industry changes, ensuring compliance across regions such as mental health billing services pennsylvania or billing services for mental health providers texas.
Focus on Patient Care
Outsourcing allows providers to dedicate more time to treatment rather than administrative tasks.
How to Choose the Right Mental Health Billing Service
Selecting the right partner is crucial for long-term success. Here are some factors to consider:
Industry Experience
Look for companies with proven experience in mental health billing service and a strong understanding of behavioral health coding.
Technology and Tools
Modern billing software improves accuracy and speeds up claim processing.
Transparency and Reporting
A reliable provider offers clear reports and regular updates on claims and revenue.
Customization and Scalability
Your billing partner should adapt to your practice size and growth needs.
Many providers compare services across regions, from a professional mental health billing company rhode island to the best mental health billing company north carolina, to find the right fit.
Regional Insights: Mental Health Billing Across the U.S.
While Columbus providers face specific challenges, it’s helpful to understand how billing varies across different states:
-
Mental health billing cleveland ohio and Columbus share similar payer policies but differ in network coverage.
-
Mental health billing services new jersey often deal with stricter compliance standards.
-
Providers seeking the best mental health billing services company new york focus on high-volume claim management.
-
Practices in need of billing services for mental health providers washington prioritize telehealth billing expertise.
-
Clinics exploring outsourcing mental health medical billing services provider in florida benefit from cost-effective solutions and scalable services.
These variations highlight the importance of choosing a billing partner familiar with multi-state regulations.
Best Practices to Improve Mental Health Billing Efficiency
Implementing the right strategies can significantly enhance billing performance:
Regular Staff Training
Ensure your team stays updated on coding and billing guidelines.
Use of Automation Tools
Automated systems reduce manual errors and improve efficiency.
Clear Documentation Standards
Maintain detailed and accurate patient records to support claims.
Frequent Audits
Conduct internal audits to identify and fix issues before they escalate.
Strong Communication with Payers
Building relationships with insurance providers helps resolve claims faster.
Why Columbus Practices Are Moving Toward Outsourced Billing
The demand for specialized billing services is increasing in Columbus. Practices are realizing that managing billing internally can limit growth and lead to revenue loss.
By partnering with experts, providers can:
-
Reduce claim rejection rates
-
Improve reimbursement timelines
-
Ensure compliance with industry standards
-
Scale operations without increasing overhead
This shift is similar to trends seen in billing services for mental health providers new york and billing services for mental health providers pennsylvania, where outsourcing has become a standard practice.
Future Trends in Mental Health Billing
The healthcare industry is evolving, and billing processes are no exception. Some trends shaping the future include:
Telehealth Billing Expansion
With the rise of virtual care, billing systems must adapt to new service models.
AI and Automation Integration
Advanced tools are improving accuracy and reducing manual workload.
Value-Based Care Models
Reimbursement is increasingly tied to patient outcomes rather than service volume.
Enhanced Compliance Requirements
Regulations will continue to evolve, making professional billing support even more important.
Conclusion
Managing mental health billing Columbus effectively requires a combination of expertise, technology, and strategic planning. With increasing complexities in insurance policies and compliance standards, relying on a structured billing approach is no longer optional.
Practices that invest in efficient billing systems or partner with experienced providers can achieve better financial outcomes, reduce administrative stress, and focus more on delivering quality patient care. Whether you are exploring mental health billing service options or comparing providers across different states, the key is to choose a solution that aligns with your practice goals.
For practices looking to streamline operations, 247 Medical Billing Services offers comprehensive support including medical billing services, medical coding services, medical billing and coding services, revenue cycle management, and credentialing services, ensuring a complete solution tailored to mental health providers.
FAQs
What is mental health billing and why is it important?
Mental health billing involves submitting claims for behavioral health services to insurance providers. It ensures that providers receive timely and accurate reimbursements.
Why do mental health claims get denied frequently?
Common reasons include incorrect coding, missing documentation, lack of prior authorization, and insurance eligibility issues.
Is outsourcing mental health billing a good option?
Yes, outsourcing helps reduce errors, improve revenue cycle management, and allows providers to focus on patient care.
How can I improve my billing process?
You can improve billing by ensuring accurate documentation, using updated coding standards, verifying insurance details, and conducting regular audits.
What should I look for in a billing company?
Look for experience, transparency, compliance knowledge, advanced technology, and the ability to scale with your practice.
Are billing requirements the same across all states?
No, billing requirements can vary by state and payer policies, which is why working with an experienced billing partner is beneficial.