The demand for accurate and efficient billing for mental health has never been higher in the USA. With increasing awareness around behavioral health, providers are seeing more patients—but also facing more complex billing regulations, payer rules, and documentation requirements. From private practices to large clinics, navigating mental health billing can directly impact revenue, compliance, and patient satisfaction.
This guide breaks down everything you need to know about billing for mental health services, including processes, challenges, solutions, and why many providers are turning to outsourcing for better results.
Why Billing for Mental Health is Different
Mental health billing is not the same as general medical billing. It involves unique coding structures, therapy session variations, time-based billing, and strict payer guidelines.
Key differences include:
- Time-based CPT codes instead of procedure-based billing
- Frequent use of modifiers for telehealth and therapy types
- Strict documentation for medical necessity
- Increased scrutiny in billing Medicare for mental health services
- Coordination between therapy, psychiatry, and medication management
Because of these complexities, many providers rely on mental health billing specialist companies to ensure accuracy and compliance.
Core Components of Mental Health Billing
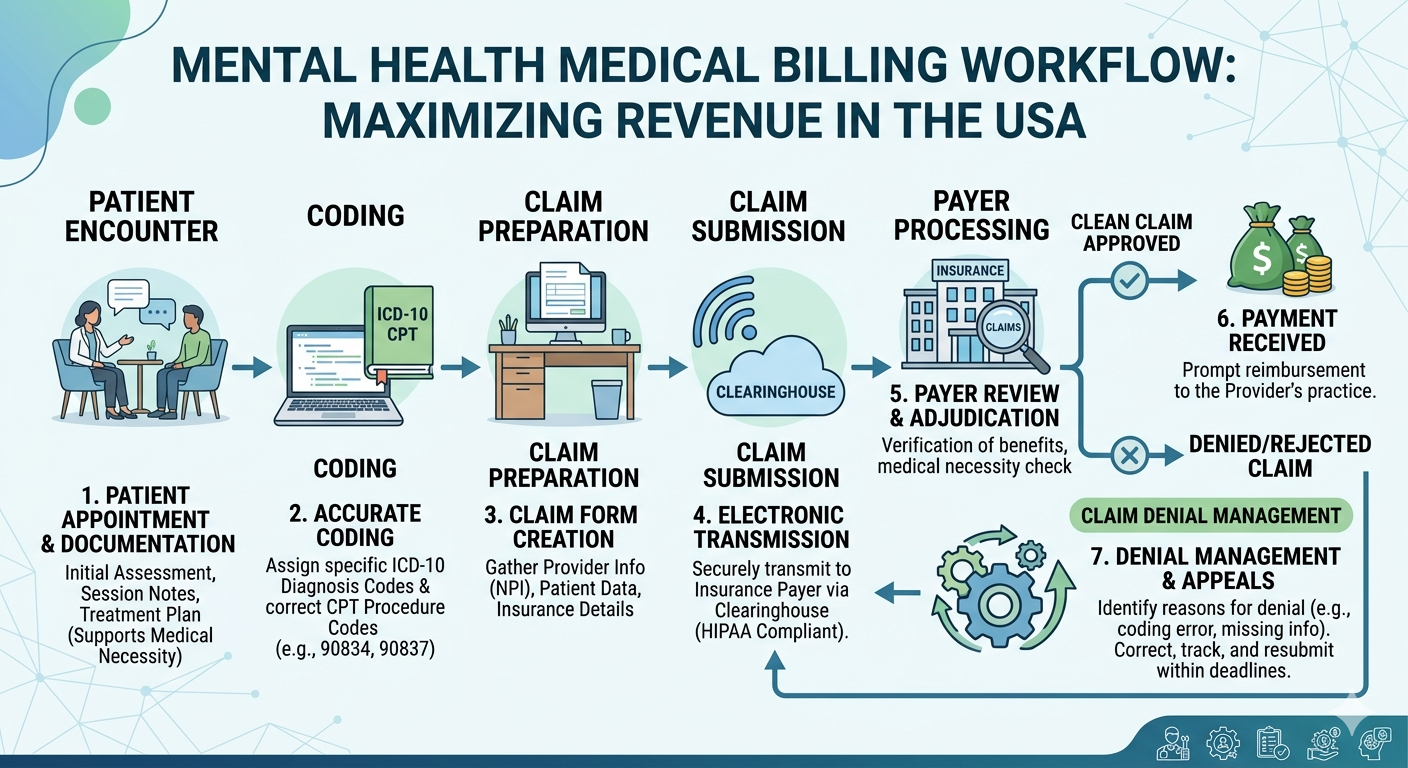
Understanding the core workflow helps providers optimize revenue and reduce errors.
1. Patient Eligibility and Verification
Before services are provided, verifying insurance coverage is critical. This ensures that billing for mental health providers is accurate from the start.
2. Accurate Coding
Coding and billing for mental health services requires proper use of CPT codes (like 90834, 90837) and ICD-10 diagnosis codes. Errors here often lead to claim denials.
3. Documentation Compliance
Payers require detailed notes to justify treatment. Incomplete documentation can delay or deny reimbursement.
4. Claim Submission and Follow-Up
Submitting clean claims and tracking them is essential. Many mental health billing services company providers specialize in reducing rejections at this stage.
5. Payment Posting and AR Management
Timely posting and aggressive follow-up ensure steady cash flow and reduce outstanding receivables.
Common Challenges in Billing Mental Health Services
Even experienced providers face hurdles when handling billing for mental health services.
- Frequent claim denials due to coding errors
- Changing payer policies and compliance rules
- Complexity in billing Medicare for mental health services
- Time-consuming administrative workload
- Difficulty managing credentialing and payer enrollment
These challenges often lead clinics to consider outsourcing mental health billing and coding to experienced professionals.
Benefits of Outsourcing Mental Health Billing
Outsourcing is becoming a preferred strategy for many practices across the USA.
Improved Revenue Cycle Performance
Outsourced billing for mental health ensures fewer errors and faster reimbursements.
Reduced Administrative Burden
Providers can focus on patient care instead of paperwork.
Expertise and Compliance
A mental health billing company stays updated with payer changes, coding updates, and compliance requirements.
Scalability
Whether you're a solo therapist or a multi-location clinic, outsourcing mental health billing supports growth without adding internal staff.
What to Look for in a Mental Health Billing Partner
Choosing the right partner is crucial for long-term success.
A best mental health billing company typically offers:
- Expertise in behavioral and mental health billing services
- End-to-end revenue cycle management
- Transparent reporting and analytics
- Credentialing support
- HIPAA-compliant systems
Top mental health billing company providers also offer customized mental health billing solutions based on practice size and specialty.
In-House vs Outsourced Billing: Which is Better?
Both approaches have pros and cons.
In-House Billing
- More control over operations
- Requires trained staff and ongoing updates
- Higher operational costs
Outsourcing Mental Health Billing
- Access to experienced professionals
- Lower overhead costs
- Faster claim processing
For many providers, outsourcing mental health billing becomes the more cost-effective and efficient option, especially when working with a cheap outsource mental health billing company that still maintains quality.
Role of Technology in Mental Health Billing
Technology plays a vital role in improving efficiency and accuracy.
Modern mental health billing services include:
- Automated claim submission
- Real-time eligibility checks
- AI-driven denial management
- Integrated EHR and billing systems
These advancements make medical billing for mental health more streamlined and less prone to errors.
Credentialing and Its Impact on Revenue
Credentialing is often overlooked but is critical for successful billing.
Mental health billing and credentialing services ensure that providers are enrolled with insurance payers and can legally bill for services.
Without proper credentialing:
- Claims may be denied
- Payments can be delayed
- Revenue loss becomes inevitable
This is why many mental health billing specialist companies include credentialing as part of their offerings.
How to Improve Your Mental Health Billing Process
Here are actionable strategies to enhance your billing performance:
- Conduct regular coding audits
- Train staff on updated billing guidelines
- Use specialized mental health medical billing software
- Monitor key performance indicators like denial rates
- Partner with experienced billing companies for mental health
Consistency and accuracy are key to long-term success.
Why Practices Are Switching to Specialized Billing Services
General billing services may not fully understand the nuances of mental health care. This is why providers prefer billing services for mental health clinics that focus specifically on behavioral health.
Specialized billing services for mental health offer:
- Better claim acceptance rates
- Faster reimbursements
- Expertise in therapy-specific coding
- Improved compliance
The best outsource mental health billing and coding services bring both efficiency and expertise to the table.
Future Trends in Mental Health Billing
The landscape of mental health billing is evolving rapidly.
Key trends include:
- Increased telehealth billing regulations
- Value-based reimbursement models
- Integration of AI in billing workflows
- Growing demand for outsourcing mental health billing
Providers who adapt to these changes will be better positioned for growth and stability.
How 247 Medical Billing Services Can Help
For practices looking to streamline operations, partnering with an experienced provider like 247 Medical Billing Services can make a significant difference. Their expertise spans medical billing services, medical coding services, and complete medical billing and coding services tailored for behavioral health.
They also offer advanced revenue cycle management services to improve cash flow and reduce denials, along with credentialing services to ensure smooth payer enrollment. This comprehensive approach helps providers focus on patient care while maintaining financial stability.
Conclusion
Billing for mental health is a complex but essential part of running a successful practice. From coding accuracy to compliance and reimbursement, every step requires attention to detail and expertise.
Whether you choose to manage billing in-house or opt for outsourced billing for mental health, the goal remains the same—maximize revenue while minimizing errors and administrative burden. With the right strategy and support, mental health providers can achieve both financial success and improved patient care.
FAQs
1. What is billing for mental health?
Billing for mental health refers to the process of coding, submitting, and managing claims for therapy, psychiatry, and behavioral health services.
2. Why is mental health billing complicated?
It involves time-based codes, strict documentation, and varying payer rules, making it more complex than general medical billing.
3. Should I outsource mental health billing?
Outsourcing mental health billing can reduce errors, improve revenue, and save time, especially for growing practices.
4. What services do mental health billing companies offer?
They provide coding, claim submission, denial management, credentialing, and full revenue cycle management.
5. How do I choose the best mental health billing company?
Look for experience in behavioral health, transparent reporting, compliance expertise, and end-to-end service offerings.
6. What is the role of credentialing in mental health billing?
Credentialing ensures providers are authorized to bill insurance companies, which is essential for receiving payments.