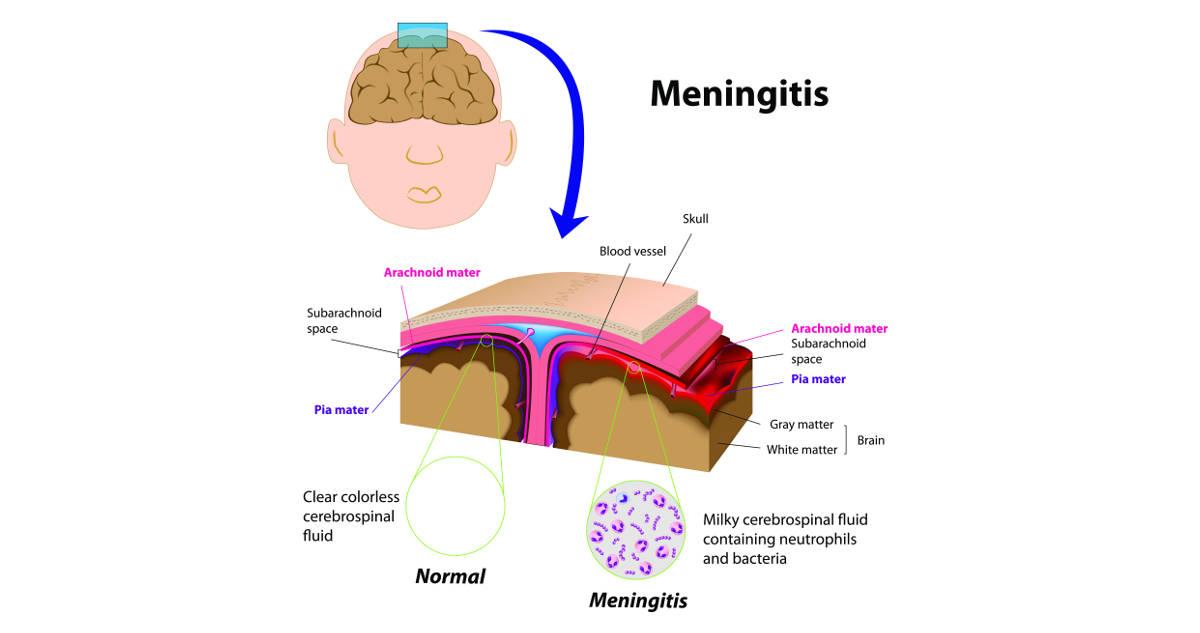
Meningitis is a serious and potentially life-threatening condition characterized by inflammation of the protective membranes (meninges) surrounding the brain and spinal cord. It can be caused by bacteria, viruses, fungi, or parasites, but bacterial meningitis is the most severe form and requires urgent medical attention. Understanding how to protect against Meningitis is critical for individuals, families, and public health systems.
Understanding the Risk
Meningitis spreads through respiratory droplets, close personal contact, or contaminated surfaces. Crowded environments such as hostels, schools, and military barracks significantly increase transmission risk. Infants, young children, elderly individuals, and people with weakened immune systems are particularly vulnerable.
The most dangerous types include meningococcal, pneumococcal, and Haemophilus influenzae type b (Hib) meningitis. Rapid progression makes prevention far more effective than treatment in reducing morbidity and mortality.
Vaccination: The Most Powerful Defense
Vaccination remains the cornerstone of meningitis prevention. Several vaccines protect against the most common bacterial strains:
- Meningococcal vaccines protect against Neisseria meningitidis
- Pneumococcal vaccines target Streptococcus pneumoniae
- Hib vaccine prevents Haemophilus influenzae type b infections
Routine immunization schedules for children include these vaccines, but adults especially those traveling or living in high-risk settings should also stay updated.
Failure to vaccinate is one of the most significant gaps in meningitis prevention strategies globally. Herd immunity also plays a key role, so widespread vaccination reduces overall transmission.
Maintain Strong Personal Hygiene
Basic hygiene practices are often underestimated but remain highly effective:
- Wash hands frequently with soap and water
- Avoid sharing personal items like utensils, toothbrushes, or water bottles
- Cover your mouth while coughing or sneezing
- Dispose of tissues properly
These measures reduce the spread of respiratory pathogens that can lead to meningitis.
Strengthening the Immune System
A robust immune system provides an additional layer of protection. Key practices include:
- Balanced diet rich in vitamins and minerals
- Regular physical activity
- Adequate sleep (7–8 hours daily)
- Stress management
Individuals with chronic illnesses or immunocompromised conditions should be particularly cautious, as they are more susceptible to infections.
Early Recognition and Medical Intervention
Despite preventive efforts, early recognition of symptoms is critical. Warning signs include:
- High fever
- Severe headache
- Neck stiffness
- Sensitivity to light
- Confusion or altered consciousness
- Nausea and vomiting
In infants, symptoms may include bulging fontanelle, irritability, and poor feeding.
Immediate medical attention can save lives. In suspected bacterial cases, antibiotics must be administered urgently.
Role of Ceftriaxone Injection in Management
While prevention is the goal, treatment readiness is equally essential. One of the most commonly used antibiotics for bacterial meningitis is Ceftriaxone.
Ceftriaxone injection is widely used because:
- It has broad-spectrum antibacterial activity
- It penetrates the blood-brain barrier effectively
- It is effective against common meningitis-causing bacteria
In emergency settings, ceftriaxone injection is often administered empirically before the exact pathogen is identified to rapidly control infection. However, misuse or overuse can contribute to antibiotic resistance, which is a growing global concern.
This underscores a critical issue: treatment alone is not sufficient. Preventive strategies must remain the priority.
Avoid Close Contact During Outbreaks
During meningitis outbreaks, minimizing exposure is crucial:
- Avoid crowded places when possible
- Maintain physical distance from infected individuals
- Use masks in high-risk environments
Public health authorities often issue guidelines during outbreaks, including prophylactic antibiotics for close contacts of infected individuals.
Environmental and Lifestyle Precautions
Certain environmental factors increase meningitis risk:
- Poor ventilation
- Overcrowded living conditions
- Seasonal variations (higher incidence in dry seasons in some regions)
Improving living conditions, ensuring proper airflow, and reducing overcrowding can significantly reduce transmission rates.
Travel Precautions
Travelers to regions with high meningitis prevalence, such as parts of sub-Saharan Africa (the “meningitis belt”), should:
- Get vaccinated before travel
- Carry medical records
- Stay informed about outbreaks
Ignoring travel-related vaccination requirements is a frequent oversight that leads to preventable infections.
Community Awareness and Education
Public education campaigns play a vital role in reducing meningitis cases. Awareness initiatives should focus on:
- Recognizing early symptoms
- Promoting vaccination
- Encouraging timely medical care
Misinformation and vaccine hesitancy remain major barriers. These are not trivial issues they directly contribute to preventable deaths.
Prophylactic Antibiotics for Close Contacts
In cases of confirmed bacterial meningitis, close contacts (family members, roommates) may receive preventive antibiotics. This reduces the likelihood of secondary infections.
However, indiscriminate use is problematic. Prophylaxis should always be guided by healthcare professionals to avoid resistance and unnecessary side effects.
Conclusion
Protecting against Meningitis requires a multi-layered approach that integrates vaccination, hygiene, early detection, and responsible medical treatment. While interventions like ceftriaxone injection are critical in managing bacterial infections, they should not be relied upon as the primary defense.
The real weakness in current global efforts lies in inconsistent vaccination coverage, delayed diagnosis, and poor public awareness. Addressing these gaps is far more impactful than focusing solely on treatment.
Prevention is not optional it is the most effective, scalable, and life-saving strategy available.