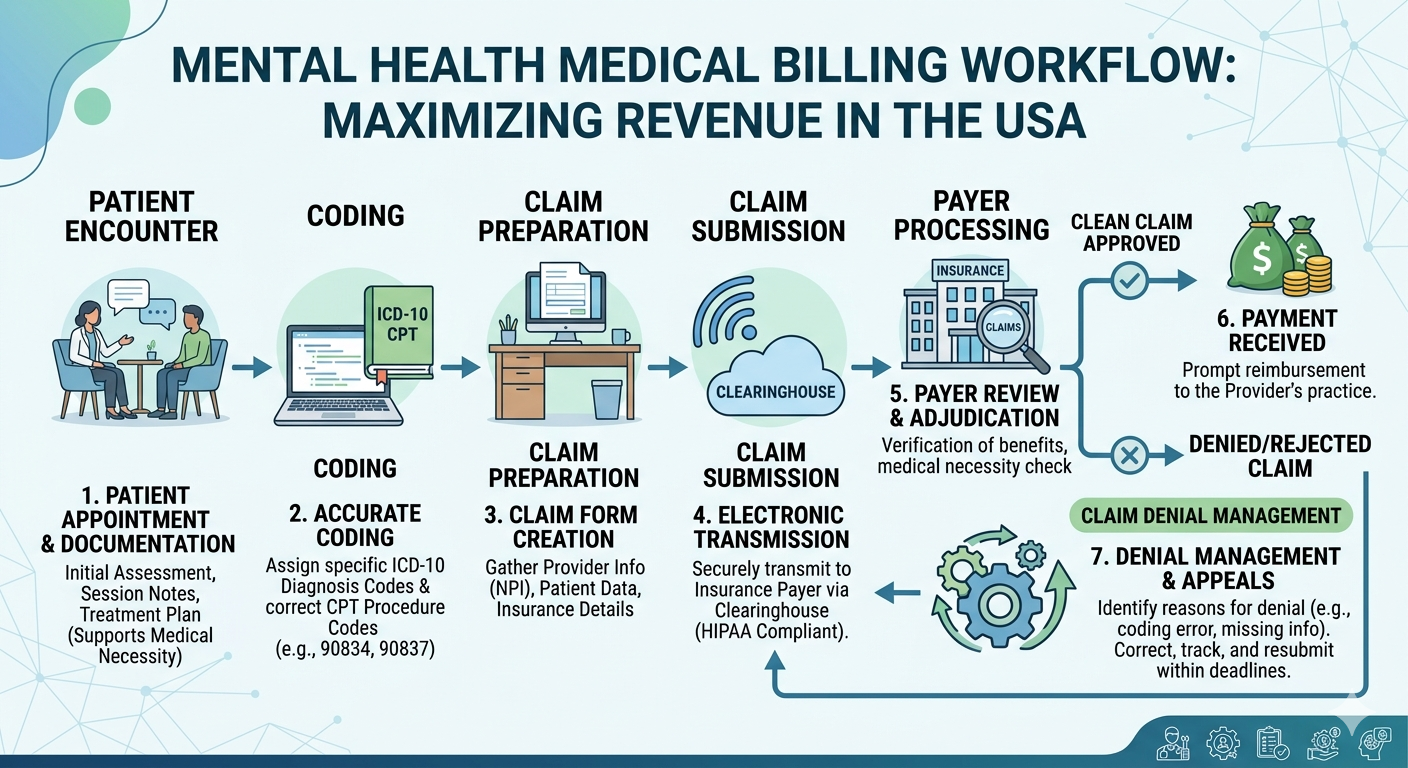
Mental health practices across the USA are growing rapidly, but so are the complexities behind getting paid. Insurance requirements, coding accuracy, and compliance standards have become more demanding than ever. For therapists, psychiatrists, and behavioral health clinics, managing billing internally often leads to delayed reimbursements and unnecessary stress.
This is where mental health billing specialist companies step in—not just as service providers, but as strategic partners helping practices stabilize cash flow and focus on patient care.
The Growing Need for Specialized Mental Health Billing
Unlike general healthcare billing, mental health billing involves unique challenges:
- Time-based CPT codes
- Frequent claim denials due to documentation gaps
- Insurance pre-authorization requirements
- Complex payer rules for behavioral health
Because of these nuances, many providers are turning to mental health insurance billing services that understand the intricacies of therapy and psychiatric billing.
A general billing team may process claims, but a mental health billing specialist ensures accuracy, compliance, and faster reimbursements.
What Do Mental Health Billing Specialist Companies Actually Do?
A professional mental health billing services agency goes far beyond submitting claims. Their role covers the entire revenue cycle:
1. Patient Eligibility & Benefits Verification
Before a session even begins, billing specialists confirm insurance coverage, co-pays, and deductibles. This reduces surprises for both providers and patients.
2. Accurate Coding
Mental health coding is precise. Incorrect CPT or ICD-10 codes can lead to denials. A mental health billing and coding company ensures every service is coded correctly.
3. Claim Submission & Tracking
Claims are submitted quickly and tracked in real-time to avoid delays.
4. Denial Management
Denied claims are not just re-submitted—they are analyzed, corrected, and appealed strategically.
5. Payment Posting & Reporting
Practices receive clear financial reports that help them understand revenue trends and performance.
This level of detail is why many providers now prefer mental health medical billing services outsourcing rather than handling billing in-house.
Why Practices Choose to Outsource Mental Health Billing Services
Outsourcing is no longer just about saving time—it’s about improving revenue efficiency.
Reduced Administrative Burden
Therapists and clinic staff can focus entirely on patient care instead of paperwork.
Faster Reimbursements
Specialized teams know payer rules, reducing claim rejections.
Cost Efficiency
Hiring and training an in-house team is expensive. Outsourced mental health billing offers a scalable alternative.
Improved Compliance
Regulations in the USA healthcare system are strict. A top outsource mental health billing company ensures HIPAA compliance and audit readiness.
Access to Expertise
You gain access to professionals experienced in behavioral health billing trends and payer updates.
Key Features of the Best Mental Health Billing Agency
Not all billing providers are equal. The best mental health billing agency typically offers:
- Dedicated account managers
- Real-time reporting dashboards
- Transparent pricing models
- Expertise in multiple mental health specialties
- Strong denial resolution processes
When selecting a mental health billing agency, practices should evaluate both technical expertise and communication quality.
Real-World Scenario: Small Therapy Practice Scaling Up
Consider a small therapy clinic in California. Initially, they managed billing internally but faced:
- 20% claim rejection rate
- Delayed payments up to 45 days
- Staff burnout
After switching to a mental health medical billing solution, they experienced:
- Reduced denials to under 5%
- Payments within 2–3 weeks
- Increased monthly revenue by 30%
This is a common outcome when practices shift to professional billing services for mental health therapists.
Mental Health Billing vs General Medical Billing
While both fall under healthcare billing, mental health has distinct differences:
| Factor | Mental Health Billing | General Medical Billing |
|---|---|---|
| Session Type | Time-based | Procedure-based |
| Documentation | Detailed therapy notes | Clinical summaries |
| Insurance Rules | More restrictive | Standardized |
| Denial Rates | Higher | Moderate |
Because of this complexity, many providers prefer mental health medical billing services tailored specifically to behavioral health.
The Role of Technology in Modern Billing
Today’s mental health billing companies are leveraging advanced tools:
- AI-assisted claim scrubbing
- Automated eligibility verification
- Cloud-based billing dashboards
- Real-time analytics
However, technology alone isn’t enough. Human expertise remains critical in interpreting payer policies and handling complex claims.
How Billing Services Support Mental Health Providers
Professional billing services for mental health providers do more than just improve cash flow—they support overall practice growth.
Better Patient Experience
Clear billing reduces confusion and improves trust.
Scalability
Practices can expand without worrying about backend operations.
Financial Visibility
Detailed reports help providers make informed decisions.
Reduced Stress
Administrative burden is significantly lowered.
Common Mistakes Practices Make Without Billing Experts
Many clinics underestimate billing complexity. Common issues include:
- Incorrect use of CPT codes
- Missing documentation
- Failure to verify insurance
- Delayed claim submission
- Poor denial follow-up
These mistakes directly impact revenue, making a strong case for mental health billing services agency partnerships.
Integrating Medical Billing and Coding Services
To truly optimize revenue, billing must work alongside coding and compliance.
A comprehensive approach includes:
- Medical billing services for claim management
- Medical coding services for accurate documentation
- Medical billing and coding services for seamless workflow
- Revenue cycle management services for end-to-end financial control
- Credentialing services to ensure providers are properly enrolled with payers
When these components align, practices achieve maximum reimbursement with minimal delays.
Why Outsourcing Is the Future of Mental Health Billing
The healthcare landscape in the USA is evolving quickly. Insurance policies change frequently, and compliance standards continue to tighten.
As a result, more practices are choosing mental health billing companies that specialize in behavioral health.
Outsourcing offers:
- Flexibility
- Expertise
- Cost savings
- Better financial outcomes
It’s not just a trend—it’s becoming the standard for modern mental health practices.
Choosing the Right Partner
Before selecting a provider, ask:
- Do they specialize in mental health billing?
- What is their claim success rate?
- How do they handle denials?
- Do they offer transparent reporting?
- Can they scale with your practice?
The answers will help identify a reliable top outsource mental health billing company.
A Practical Look at Long-Term Value
Think beyond immediate cost savings. The right billing partner contributes to:
- Long-term revenue growth
- Operational efficiency
- Regulatory compliance
- Practice expansion
This is why many clinics invest in mental health medical billing services outsourcing as a strategic decision rather than an operational expense.
Supporting Your Practice with the Right Expertise
In today’s competitive healthcare environment, aligning with a provider that understands both billing and compliance is essential. Companies like 247 medical billing services offer integrated support across:
- medical billing services
- medical coding services
- medical billing and coding services
- revenue cycle management services
- credentialing services
This kind of holistic approach ensures that mental health practices are not only getting paid—but getting paid accurately and on time.
Conclusion
Mental health providers play a critical role in improving lives, but financial stability is equally important for sustaining that impact. Partnering with experienced mental health billing specialist companies allows practices to streamline operations, reduce errors, and improve revenue.
As billing complexities continue to rise in the USA, outsourcing to a specialized mental health billing agency is no longer optional—it’s a smart, future-focused move.
FAQs
1. What are mental health billing specialist companies?
They are specialized service providers that handle billing, coding, and insurance claims specifically for mental health practices, ensuring accurate and timely reimbursements.
2. Why should I outsource mental health billing services?
Outsourcing reduces administrative workload, improves claim accuracy, speeds up payments, and ensures compliance with insurance regulations.
3. How do mental health billing services differ from general medical billing?
Mental health billing involves time-based codes, stricter documentation, and more complex insurance requirements compared to general medical billing.
4. What should I look for in a mental health billing agency?
Look for experience in behavioral health, transparent reporting, strong denial management, and end-to-end revenue cycle support.
5. Can billing services help small therapy practices?
Yes, even small practices benefit significantly through reduced denials, faster payments, and improved operational efficiency.
6. Do billing companies also provide coding and credentialing support?
Many providers offer complete solutions, including medical coding, credentialing, and revenue cycle management for comprehensive support.